The UK, one of the worst hit European countries, has given emergency approval to the vaccine to help control the spread of COVID19. As early as Monday, the elderly and health care workers will start receiving the vaccine in London. The EMA, on the other hand, won’t review the vaccine until the end of December.
In normal circumstances, a 28-day delay would not have the potential for dire health consequences. But COVID19 is currently spreading the worst it ever has in Europe and the U.S. Thousands of lives could be saved by emergency approval of the vaccine. Recognising this, the U.K. has decided to approve the vaccine as fast as possible, despite the risk of undesirable health effects that the vaccine may cause.
This raises a very important regulatory question: If the vaccine is proven safe, what are consequences on human health of a delay? The EMA is implicitly stating that the lives lost as a result of not recognising the U.K. approval are worth extra safety gained by a more thorough review of current COVID19 vaccine candidates.
I don’t have a model of the spread of COVID19 in the EU at hand, but I do have a model for the U.S. It’s worth noting that COVID19 is currently killing nearly 5,000 people a day in the EU – even more than the U.S. per capita, suggesting an even more urgent need for a vaccine in Europe.
My model for the U.S. has the following assumptions based on statements by Doctor Fauci, Moderna and Pfizer:
- Vaccine distribution begins originally on December 15th in the baseline scenario vs January 12th in the late scenario.
- 50 million vaccines distributed in the first month and 75 million each month after
- Risk profiles by age group are based on CDC data. Most of the health benefit is therefore captured when those over 70 are vaccinated – they are at 1800x the risk of death compared to children and more than 100x at-risk compared to those from 50-70 years old. EU risk profiles are basically identical.
- The vaccine is distrubuted based only on the risk profile of age subgroups. The EU, UK, Canada and U.S. have said they will generally follow this approach.
- The vaccine eventually reaches an 80% coverage rate and has a 90% efficacy in preventing hospitalisations and deaths.
- The effective-r value will remain in the range of effective-r values over the past few weeks. This will mean no Christmas surge in infections that would make late approval of a vaccine even more deadly.
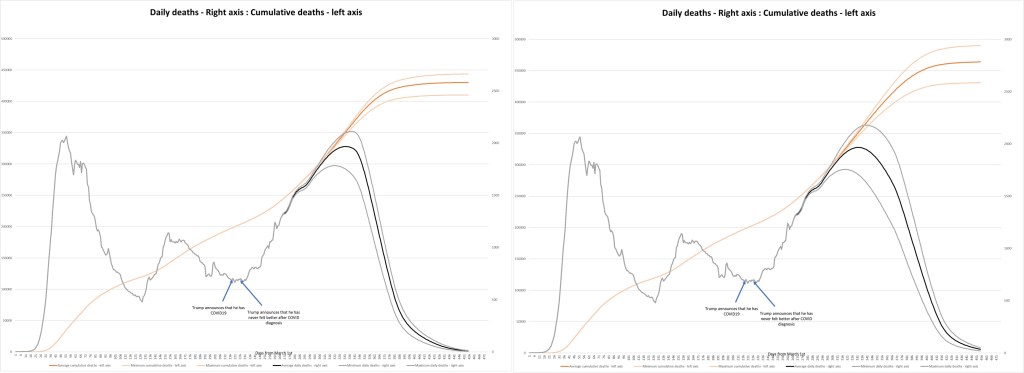
Based on this relatively simple model, in the baseline scenario with vaccine, the U.S. would reach up to 450K deaths by the end of the epidemic – a figure broadly in line with IHME forecasts, which hasn’t yet factored in a readily available vaccine. However, a vaccine delay of just 28 days raises that figure to just under 500K or a 10% increase.
It’s difficult for me to understand how the EMA could view 10% more deaths a worthwhile trade-off to better assess the safety and efficacy of a vaccine.








You must be logged in to post a comment.